What Is Fentanyl?
Fentanyl is a prescription drug for pain relief that is also made, sold, and used illegally. It is like morphine but up to 100 times more potent.
Fentanyl is an incredibly powerful opioid. It has become the most widely used synthetic opioid in medical practice.
Opioids are a family of drugs naturally found in the poppy plant. Some opioids are entirely natural, made from the plant directly, and others are made in a lab. Several are semi-synthetic, but fentanyl is fully synthetic, completely made in a lab using the same chemical structure.
Synthetic opioids, including fentanyl, are the most common drugs connected to overdose related deaths in the United States.
By binding to the brain’s opioid receptors, responsible for controlling pain and emotions, fentanyl changes how you respond to pain. As a result, it effectively blocks your nervous system from sending pain signals to the brain.
Fentanyl Street Names
Common street names for illegally used fentanyl include:
- China girl
- China white
- Apache
- Dance fever
- Birria
- Jackpot
- Murder 8
Brand Names
In prescription form, fentanyl is available in the following brand names:
- Actiq
- Duragesic
- Sublimaze
- Abstral
- Fentora
- Subsys
- Lazanda
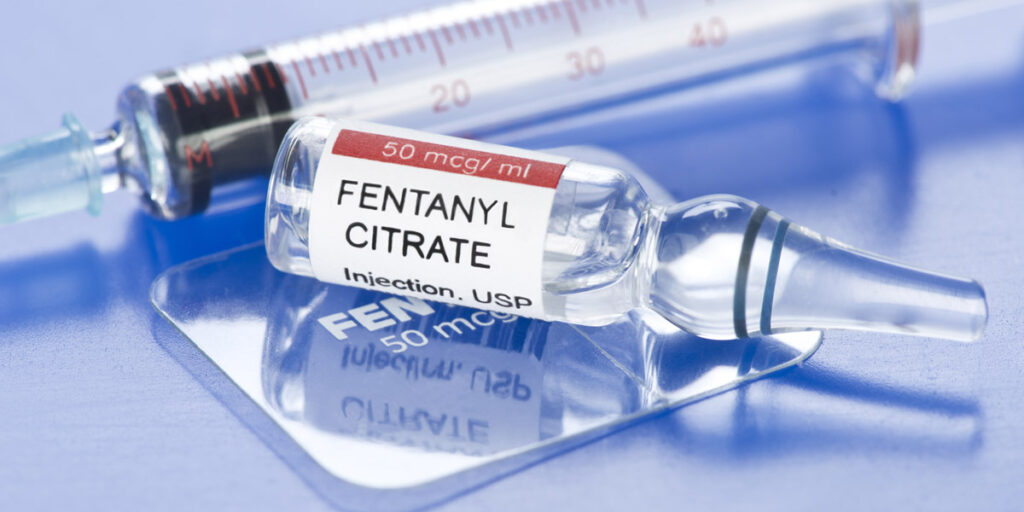
What Is Fentanyl Used for?
Like morphine, fentanyl uses are varied. It is most commonly used to manage severe pain, especially after surgery and chronic pain in patients with a physical tolerance to opioids.
In 1968, fentanyl was approved for general anesthesia and is still widely used today. Because of its quick delivery and short effects, it is particularly effective in the use of anesthesia.
Fentanyl is used as a pre-medication in procedures, specifically those anticipated to cause discomfort, and for pain control during recovery in the hospital. Furthermore, it is used to treat epilepsy and pain in cancer patients at least 18 years old.
Forms
When prescribed by a doctor, fentanyl is available in many forms. It is produced as a shot, skin patch, nasal spray, dissolvable oral film, lozenges, oral tablets, and a lozenge on a handle, also known as a fentanyl lollipop.
However, when acquired illegally, it is most often found as a powder. Fentanyl powder can be made into pills or put in nasal sprays. The liquid form is commonly placed in eye droppers, blotted on paper, or put on candy.
Fentanyl Patch
Fentanyl patches deliver powerful, continuous opioid medication through your skin over 72 hours, making them effective for chronic pain when you’re already tolerant to opioids. You’ll face serious risks including respiratory depression, sedation, and potentially fatal overdose, especially if you’re opioid-naïve or using them for acute pain. The patch’s fixed release prevents dose adjustments, and fentanyl stays in your system hours after removal. Understanding proper use and dangerous drug interactions can help you stay safe.
A fentanyl skin patch, also known as a transdermal patch, manages and treats chronic pain from a terminal illness, such as cancer. In addition, it is valuable for patients who can’t tolerate high doses of oral opioids and those who are opioid-tolerant and are already receiving other pain medications that may not be sufficient.
Who Should Use Fentanyl Patches for Chronic Pain?
Fentanyl patches deliver powerful pain relief for specific patient populations who meet strict medical criteria. You’re a candidate if you’ve demonstrated opioid tolerance through prior treatment equivalent to at least 60 mg daily oral morphine for one week. This transdermal delivery system works best when you have persistent moderate to severe chronic pain requiring continuous around-the-clock opioid analgesics.
Your doctor may prescribe fentanyl patches if you experience intolerable side effects from oral opioids, including severe nausea or grade III+ constipation. Cancer patients with stable opioid demand benefit from 72-hour analgesia unaffected by gastrointestinal issues. Patients with malignant intestinal obstruction experiencing moderate or severe cancer pain are also ideal candidates, as the transdermal route bypasses the digestive system entirely. Because fentanyl considerably affects your CNS and respiratory system, you must understand that these patches are contraindicated if you’re opioid-naive with non-cancer pain. There is also significant danger with too rapid dose escalation, which can cause serious harm or fatalities even in long-term opioid users. If you experience any adverse reactions while using fentanyl patches, you can report them to the FDA MedWatch program to help ensure ongoing product safety.
Fentanyl patch doses are made to deliver the medication at a constant rate and are available in several doses: 12, 25, 50, 75, and 100 micrograms per hour.
How Fentanyl Patches Deliver Steady Pain Relief
Understanding who qualifies for fentanyl patch therapy naturally leads to examining how these delivery systems actually work to maintain consistent pain control.
When you apply a fentanyl patch, the medication moves from the adhesive layer through your stratum corneum into your bloodstream. Your skin absorbs fentanyl at a 92-94% rate through micropores, where capillaries deliver it systemically. After 24 hours, your epidermis forms a secondary reservoir, sustaining steady release.
Fentanyl patches create a skin reservoir that delivers medication steadily into your bloodstream over 24 hours.
You’ll reach effective serum levels within 6-12 hours, with steady state occurring between 12-24 hours. Peak concentrations develop 24-72 hours post-application. The FDA notes this sustained delivery provides 30% lower constipation and sedation rates compared to oral morphine.
However, the same lipid solubility enabling effective transdermal absorption contributes to respiratory depression and overdose risk, requiring careful monitoring throughout treatment.
Also, fentanyl’s half-life is 17 hours. That means it takes blood levels 17 hours to drop half of the drug from its system after the patch is removed. Thus, drug interactions with other opioids are still a risk after the patch is off.
In addition, many people using fentanyl patches do not equate it to taking medication. Therefore, extra caution must be taken when another drug is being considered for administration. For example, a dentist that sedates a patient without identifying the presence of the patch can be life-threatening.
How to Apply and Replace Your Fentanyl Patch Safely
Proper patch placement directly affects how well your fentanyl absorbs into your bloodstream, so you’ll want to choose a flat, hairless area on your chest, back, upper arm, or side of your waist. Select only intact skin that’s free from cuts, irritation, or scarring, and avoid areas that bend or move frequently. You’ll replace your patch every 72 hours, rotating to a different site each time to protect your skin and maintain consistent medication delivery.
Choosing the Application Site
When you’re ready to apply your fentanyl patch, selecting the right location on your body directly impacts how well the medication absorbs and how securely the patch stays in place.
For adults, recommended sites include your upper arm, chest, back, sides of your waist, or flank. Children or cognitively impaired patients should use the upper back to prevent tampering. The inner thigh offers another flat, hairless option.
You’ll need to avoid skin folds, wrinkled areas, and highly mobile regions. Stay away from radiation-exposed or sensitive skin. If you’re using multiple patches, separate them to prevent edge overlap.
Rotate your application sites regularly to minimize irritation. Given fentanyl’s dependence potential, consistent and correct placement guarantees steady medication delivery while reducing complications from improper absorption.
Patch Replacement Schedule
Because fentanyl patches release medication over a specific timeframe, you’ll need to replace yours every 72 hours, or every 3 days, unless your healthcare provider directs otherwise. Some patients require replacement every 48 hours due to individual absorption differences, so follow your provider’s specific instructions.
When it’s time for a new patch, remove the old one and apply the replacement to a different skin area. Wait at least 3 days before reusing the same location. Keep a consistent schedule by noting your application times.
If you miss a dose, apply the patch as soon as you remember. However, if it’s nearly time for your next scheduled application, skip the missed dose, never apply extra patches. Avoid placing direct heat sources over your patch, as this increases absorption and overdose risk.
Fentanyl Patch Side Effects Compared to Oral Opioids
While fentanyl patches and oral opioids both provide effective pain relief, they differ considerably in their side effect profiles. Transdermal fentanyl bypasses your digestive system entirely, which reduces gastrointestinal complications markedly.
Transdermal fentanyl skips your gut entirely, dramatically cutting the digestive side effects that plague oral opioid users.
Clinical evidence demonstrates these key differences:
- Constipation rates drop dramatically, you’ll experience 16-22% incidence with patches versus 28-46% with oral morphine
- Nausea and vomiting decrease substantially, only 2-9% of patch users report nausea compared to higher rates with oral formulations
- Sedation occurs less frequently, randomized trials show drowsiness increases with morphine but not transdermal fentanyl
If you’re struggling with severe nausea from oral opioids, your doctor may recommend switching to fentanyl patches. However, you must understand that respiratory depression remains a serious risk, particularly if you’re opioid-naive.
Adverse effects that may need medical attention involve:
- Seizures
- Hallucinations
- Fever
- Sweating
- Shivering
- Loss of coordination
- Hives
- Rash
Medications That Increase Fentanyl Overdose Risk
Several medication categories dramatically increase your risk of fatal overdose when combined with fentanyl patches. CNS depressants pose the greatest danger, alcohol, benzodiazepines, and GHB can cause respiratory failure and death when mixed with fentanyl. Other opioids, including heroin and oxycodone, create additive effects that overwhelm even tolerant individuals.
Stimulants like cocaine and methamphetamine strain your heart through opposing cardiovascular effects. You’re also at risk if one drug wears off before the other, triggering delayed overdose.
Xylazine, increasingly found in street drugs, causes life-threatening breathing depression and dangerously low blood pressure alongside fentanyl. The White House has declared this combination an emerging threat.
SSRIs and MAOIs carry rare but serious interaction risks, including serotonin syndrome. Always disclose all medications to your prescriber before starting fentanyl therapy.
Why Fentanyl Patches Are Unsafe for Acute or Mild Pain
Understanding dangerous drug interactions represents only part of fentanyl patch safety, you must also recognize when these patches shouldn’t be used at all.
Fentanyl patches are FDA-approved exclusively for opioid-tolerant patients with chronic pain requiring continuous relief. They’re contraindicated for acute or postoperative pain because their pharmacokinetics create dangerous mismatches, pain resolves faster than fentanyl clears your bloodstream, risking fatal overdose.
Fentanyl patches are designed for chronic pain in opioid-tolerant patients, never for acute or postoperative pain management.
Why fentanyl patches don’t work for short-term pain:
- Serious respiratory depression peaks within 24-72 hours, potentially killing you before acute pain naturally subsides
- The 72-hour fixed release prevents dose adjustments when your pain fluctuates or disappears
- Prolonged elimination means breathing problems persist hours after patch removal
Manufacturers explicitly warn against postoperative use. For acute pain, your healthcare team should use multimodal analgesia with adjustable, short-acting medications instead.

Is it Dangerous?
Because fentanyl is so powerful, it takes only a little to produce a high, making it a cheaper option for drug dealers. They mix heroin, cocaine, meth, and MDMA with it, creating an especially hazardous situation because people are unaware that fentanyl has been added.
Fentanyl is more potent than morphine and heroin. A 3-milligram dose of fentanyl is enough to kill an average-sized adult. Sometimes it is disguised as potent heroin, creating an even higher likelihood of an overdose.
Fentanyl Overdose
As mentioned above, since dealers like to mix fentanyl into other drugs to increase profits, it is hard to know which drug is causing the overdose; thus, broadening the difficulty of knowing which medication to reverse the drug overdose. And since fentanyl is stronger than any other opioid, it might require several doses of an opioid antagonist, a medication that reverses an opioid overdose.
Fentanyl Abuse
After taking a drug continuously, your brain adapts to the substance, reducing sensitivity, making it challenging to feel satisfaction from anything other than that. This is how tolerance happens, taking larger doses or using more frequently to get the same effects. This is especially dangerous with fentanyl.
The main danger of fentanyl abuse is respiratory depression, slowed or stopped breathing, just like any other opioid. However, the increased risk of overdose with fentanyl lies in a mix of its exceptionally high potency and users’ tendency not to be aware of its presence.
Fentanyl Addiction Help in Los Angeles
Individuals addicted to fentanyl can suffer severe withdrawal symptoms within hours after the drug was taken. These symptoms can be extremely uncomfortable and may be the reason you can’t stop using fentanyl.
Northridge Addiction Treatment Center understands the necessity for a comfortable and serene, medically supervised detox program. Our facility in the heart of the Los Angeles valley gives you the environment and support needed to work on yourself. You won’t have to take this journey on your own. NATC specialists will help you every step of the way, starting from enrollment all the way to successfully joining our alumni program. Call to speak with an admissions specialist today.
Learn more about our treatment programs and our medication assisted treatment program for opioid use disorder.
Frequently Asked Questions
Can I Swim or Shower While Wearing a Fentanyl Patch?
Yes, you can swim and shower while wearing a fentanyl patch. These patches are waterproof and remain effective during normal water exposure with cold or lukewarm water. However, you must avoid hot tubs, hot baths, and saunas, as heightened temperatures increase fentanyl absorption and can cause overdose. After swimming or showering, check that your patch remains properly adhered and dry the surrounding skin completely.
What Should I Do With Used Fentanyl Patches After Removal?
After removing your fentanyl patch, fold it in half with the sticky sides together. The FDA recommends flushing used patches down the toilet immediately to prevent accidental exposure to children or pets. Alternatively, you can place the folded patch in a tamper-proof, childproof container and return it to your pharmacy. Always wear gloves when handling used patches and wash your hands thoroughly afterward.
How Long Does It Take for a Fentanyl Patch to Start Working?
You’ll typically start feeling the effects of a fentanyl patch around 12 hours after application, though full analgesic relief may take up to 24 hours. The medication builds up in your skin before entering your bloodstream, which explains this delay. Your doctor will likely prescribe a short-acting opioid to manage pain during this initial period. Factors like your age and skin permeability can affect how quickly you respond.
Can Heat Exposure Affect How Much Fentanyl My Patch Releases?
Yes, heat exposure markedly increases fentanyl release from your patch. When you apply heat sources like heating pads, electric blankets, or hot baths to the patch area, your skin absorbs the medication faster, potentially tripling blood levels within the first four hours. This rapid absorption raises your risk of serious side effects or overdose. You should avoid direct heat sources, saunas, and strenuous exercise while wearing your patch.
What Happens if My Fentanyl Patch Falls off Before 72 Hours?
If your fentanyl patch falls off before 72 hours, you should dispose of it properly and apply a new patch to a different, dry skin area. Leave the replacement patch on for the full 72 hours. Contact your doctor to report the early removal. Even after the patch falls off, fentanyl continues absorbing from your skin for hours, so watch for signs of overdose like slow breathing or extreme drowsiness.




