What Are the Dangers of Using Shared Needles?
Drug Injection Use
All drug use poses a risk, but injection users sharing needles, syringes, and other injecting equipment are some of the most at risk for infectious diseases and long-term health problems.
As the opioid crisis and drug addiction in the United States continue to spread, many people inject drugs such as heroin, prescription medications, and amphetamines directly into their veins for a quicker high.
Intravenous drugs (IV drugs) require tools to prepare and inject, which can be hard to get.
There are many reasons people will reuse and share needles, including availability issues, the stigma of addiction, and lack of knowledge associated with the risks needle sharing can pose.
Many people who inject drugs are unaware that sharing needles contributes to human immunodeficiency virus (HIV) and hepatitis C transmission and infection.
Learning to avoid sharing needles, care for wounds, and recognize the signs of disease are essential steps in the battle against addiction and public health threats related to IV drug use.
What Does Sharing Needles Mean?
Sharing needles means two or more people use the same syringe, often multiple times, to inject drugs intravenously.
Needles are the most commonly reused drug paraphernalia, especially among people lacking access to clean needles or education about the dangers of needle sharing.
Injection users face an increased risk of infectious diseases caused by sharing needles and syringes.
When intravenous drug users prepare drugs such as heroin or prescription opioids to inject, they mix them with sterile water in a clean container called a “cooker” for heating drugs, fresh cotton to filter the mixture through, and a sterile needle to inject themselves.
When people discuss sharing needles, it typically includes sharing other paraphernalia, which can contribute to transmitting bloodborne diseases.
Many users who use new or sterilized needles have admitted to sharing other equipment with people.
Needle Sharing Statistics
Tracking the health of intravenous drug users is an integral part of developing public health and harm reduction programs.
- The World Health Organization (WHO) estimates that 11 million people inject drugs worldwide.
- Out of 11 million intravenous drug users, approximately 40% have contracted the hepatitis C virus.
- At any given time, 1.4 million people who inject drugs live with HIV.
- Globally 10% of newly reported HIV cases are attributed to drug use injections.
- According to the Centers for Disease Control (CDC), an estimated 1.18 million people have HIV in the United States.
- Roughly 36,000 Americans will receive an HIV diagnosis each year.
- Of new HIV cases in the United States, young people between 13 to 24 years old will account for 21%.
These statistics only relate to injecting drugs intravenously; they do not account for secondary infections and viruses or sexually transmitted infections caught through other circumstances surrounding risky drug use and behavior.
Gathering data and statistics about people who inject drugs is a challenge for researchers because many people are ashamed or embarrassed about their drug usage and give inaccurate answers.
When health care professionals are unaware of a patient’s drug use, they often won’t test for infectious diseases associated with injecting drugs like HIV and hepatitis C.

Can You Share Needles With a Clean Person?
If possible, you should never share needles, even if a person claims they are clean. You cannot take someone’s word for it. Many drug users do not know or believe they are at risk for contracting or transmitting diseases and do not regularly get tested.
The CDC states that HIV-infected blood can survive up to 42 days in a used syringe, meaning that someone could contract it after a negative test and transmit HIV unknowingly over a month later.
Sharing needles with a clean person, as in someone without HIV and hepatitis B or C, only reduces the risk of contracting a disease if none of the other drug equipment is tainted or shared.
Sharing needles and equipment still increases the risks of other bacterial infections and needle-related injuries.
Needles become dull very quickly, which leads to complications and injuries when injecting a drug; this is just one more reason to never share needles regardless of health status.
Drug Injection Side Effects
Injecting drugs intravenously or “shooting up” has additional side effects and complications besides the risks of bloodborne diseases.
After long-term or heavy injection drug use, many users cannot find a suitable vein and will start injecting directly into their muscles or under the skin.
Some of the side effects of drug injection include:
- Bruising
- Collapsed veins
- Track marks
- Skin infections
- Abscesses or swollen, puss-filled wounds
- Swelling of limbs due to lack of blood flow
- Joint pain
- Fevers
- Diseases
Some of these side effects will resolve if the user switches injection sites or stops injecting drugs altogether; however, some can lead to infections and more severe complications.
Always seek medical advice if you are concerned about a wound or side effects you haven’t experienced previously.
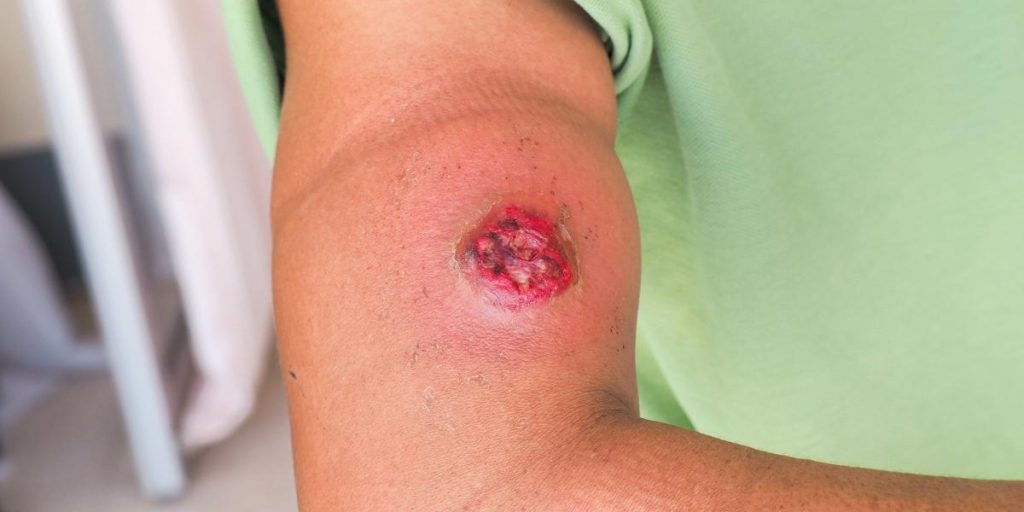
What Diseases Are Caused by Sharing Needles?
Injecting drugs exposes people to many infectious diseases, some curable and some that become life-long conditions. Some diseases have minimal symptoms for years, and others become life-threatening right away.
Using sterile equipment, not sharing needles or paraphernalia, practicing safe sex, and getting tested regularly are essential steps to reducing disease risk. However, recovery and abstinence are the only 100% proven ways to avoid diseases and prevent HIV and hepatitis C transmission to others.
The infections and diseases IV drug users are at risk of contracting include:
- Cotton fever – reused cotton filters breed a bacteria that can lead to flu-like symptoms; people with allergies are more susceptible
- Cellulitis – bacterial infections that cause the cells to become painful and swollen
- Necrotizing Fasciitis – the “flesh-eating disease,” can rapidly spread and lead to death
- Wound or injection botulism – affects the respiratory and nervous system leading to paralysis and death
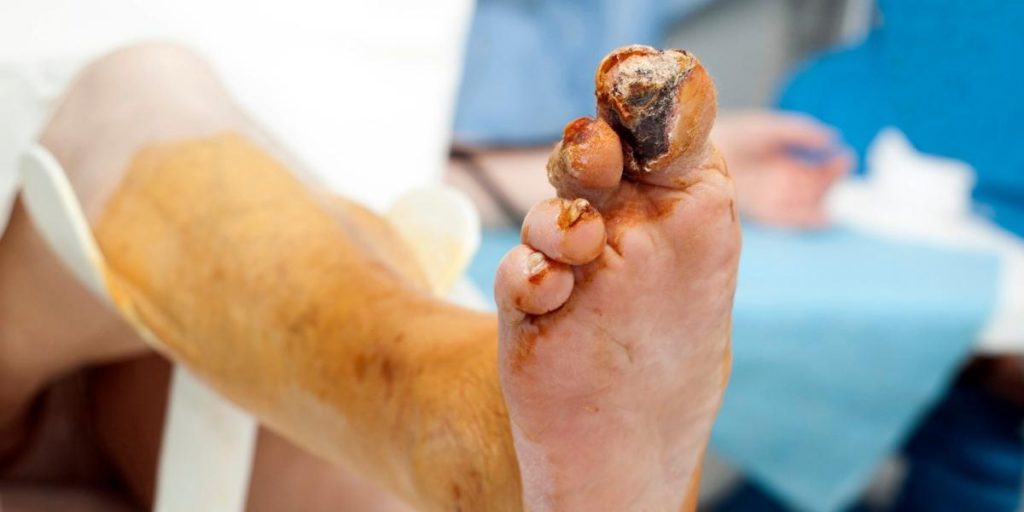
- Gangrene – an infection that causes a loss of blood flow and tissue death, can lead to amputation or death
- Tetanus – or “lockjaw,” attacks the muscles and causes them to swell and lock up
- Infective endocarditis – bacteria gathers on the heart valves, enters the bloodstream, and leads to life-threatening complications
- Hepatitis B – an incurable liver disease that can lead to liver cancers and death; it is 5-10 times more contagious than hepatitis C
- Hepatitis C – an infection that can lead to liver failure and death; there is a cure, but many people actively using drugs cannot adhere to the strict medication schedule, which results in a chronic condition
- Human immunodeficiency virus (HIV) – attacks the body’s immune system and can lead to acquired immunodeficiency syndrome (AIDS)
- Syphilis – because many users engage in risky sexual behavior while using or to support their habit, studies have shown that syphilis is frequently co-occurring in HIV positive IV drug users
- Acquired immunodeficiency syndrome (AIDS) – the final progression of HIV results in a severely damaged and weakened immune system, allowing other illnesses to overtake the body and often resulting in death
Many of these diseases do not have a cure yet, but with early intervention and ongoing treatment, most of them can be managed and are not a death sentence.
Harm Reduction Strategies
Intravenous drug use is considered a public health crisis and many governments and communities invest in harm reduction and prevention services for IV drug users.
Harm reduction is a multipronged approach that focuses on reducing the risk of HIV and hepatitis C transmission, providing users education, resources, and information about staying safe and accessible healthcare, mental health, and addiction treatment options.
Many harm reduction centers offer multiple prevention strategies and can provide referrals for other services.
Some of the most common harm reduction strategies include:
- Syringe Service Programs— sometimes just called needle exchange or syringe programs, users can access sterile equipment and safely dispose of their used paraphernalia; information about sterilizing equipment when necessary is also available.
- Safe Injection sites— staff members teach users safe injection practices to avoid harm and trauma, provide first aid for existing wounds and infections, administer HIV testing, and screen for other infectious diseases.
- Narcan distribution and overdose prevention— users and their friends and family can receive Narcan (naloxone) and education on administering it and other ways to prevent, recognize, and treat opioid overdoses.
- Treatment program and therapy referral— for users ready to enter recovery and quit using drugs, harm reduction centers can provide information and referrals for programs to help them achieve recovery.
Tips to Inject More Safely
The Minnesota Department of Health (MDH) offers simple tips to help drug users inject more safely, including:
- Use a needle once. Don’t share needles with other people, and don’t recycle or reuse your needle. Needles tend to dull after one attempt to inject. If you miss your vein, stick again with a clean, fresh needle.
- Alternate your injection sites. Scar tissue starts to grow under a repeatedly used injection site. It’s crucial to change the location on the body and the side of the injection.
- Wash the injection site with soap and water.
- Don’t share. Don’t share needles, cookers, wipes, or tourniquets. All of these supplies run the risk of passing infectious diseases.
- Always try to use with someone. Take turns observing for signs and symptoms of an overdose.
- Prepare and make a safety plan. Stock up on syringes, cotton, sterile water, and various needle sizes.
- Keep naloxone readily available and try to carry several doses. Tell friends and family that you have naloxone if there is an emergency.
Simple safety tips and harm reduction strategies are integral to staying alive for people battling drug and alcohol dependency and substance abuse disorders. Still, it is not the same as recovery.
Drug Addiction Treatment
Intravenous drug use can make you feel like an outcast or like you have hit rock bottom, but there is always a way forward.
At Northridge Addiction Treatment Center, our passionate and expert addiction treatment specialists firmly believe that everyone can find a meaningful path to recovery. We are eager to help with an abundance of acceptance and support.
Surrounded by the serene beauty of Los Angeles’ San Fernando Valley, you have the privacy and support to begin healing and overcoming your addiction.
NATC is an empowering and comfortable residential treatment facility featuring healthy, chef-catered meals, flat-screen TVs in each room, and a relaxing pool and hot tub area.
We understand that the thought of withdrawal can be overwhelming. NATC ensures your comfort and safety with onsite medical detox, followed by evidence-based treatment programs tailored to your unique needs.
Behavioral therapies such as cognitive-behavioral therapy (CBT), dialectical behavior therapy (DBT), and support groups will equip you with the skills to regain and maintain your mental and physical well-being for a lasting, sustainable recovery.
Our admissions team looks forward to answering your questions and concerns. Reach out now to take the first steps toward your path to recovery.
Find Meaningful Recovery
Our caring and compassionate specialists are eager to help you comfortably navigate this journey to recovery. Our individualized treatment plan, programs, and therapies may be a perfect match for you or your loved one. Let us assist you in living the happy life you deserve. It starts with a phone call.




